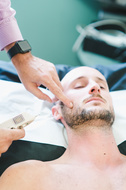
A 15 year old girl developed R shoulder pain one year ago after sleeping on it weird. Pain is constant and unable to raise hand above shoulder height (for instance raising her hand in school to ask a question).
3 months after the onset she had a diagnostic ultrasound which found a small supraspinatus tear (rotator cuff muscle). She then had 24 physical therapy visits over 12 weeks with no improvement. 2 months later she had a shoulder MRI - this did NOT show a supraspinatus tear.
11 months after initial onset the patient was referred to me. Pain was still constant (10/10 on VAS) EXSTORE exam was as follows:
•unable to flex shoulder above 90 deg on R
•scapular stability (serratus anterior) on R is inhibited
•during testing of serratus anterior upper trapezius is in spasm
•c spine ROM to the left is 45 deg
•patient cannot do any pushup or modified pushup in school gym class.
•Patient is afraid of needles.
TREATMENT
•the patient agrees to only one needle with some convincing from her mother but does NOT agree to Pointer Plus stimulation.
•I insert needle into serratus anterior with a twitch response - and leave for 30 seconds then follow up with some manual fascial release to the mid axillary line.
RESULT
The patient was off for Christmas for 2 weeks and when she returned she reported her shoulder was 80% less painful (2/10 of VAS)
•shoulder flexion improved to 170 degrees and the scapular stability was 100% stable on EXSTORE re-exam. Her c spine ROM was now 80 deg rotation bilateral.
DISCUSSION
Being specific with your assessment will pay dividends. Take diagnostic imaging into consideration but do not lean on it - do a functional exam. For a joint to move you need two things: muscles to stabilize the joint being moved and muscles to do the moving. This is why learning to assess and treat the serratus anterior is non-negotiable when aspiring to become consistently proficient in treating shoulder and neck dysfunction. This girl had 24 visits with another therapy. 24 visits! Clearly those therapists didnt know what they didnt know. We have the tools and its easier than you think folks.
Thank you to @susan_beck for showing me this
Neat little feature on the Locals Phone app.
Bookmarks Help you save post and videos that you want to go back to later.
Give this a read after you watch the video: https://pmc.ncbi.nlm.nih.gov/articles/PMC7689775/
You can save 25-50% on an in-person seminar for 2026 while you build your on-line library!
Here's how:
• Spend $500 on digital classes and get 25% off an in-person class
• Spend $800 on digital classes and get 50% off an in-person class
Excludes the Clinical Intensive
Coupon code will be emailed to you after digital order is completed
This includes webinars, online courses, bundles - everything that is on sale right now!
Sale ends May 30th at midnight.
Click here to start shopping: https://aseseminars.com/on-demand-education/?v=34f435c6b599















